![]()
Ciências Biofarmacêuticas; Biomed Biopharm Res., 2021; 18(2):238-251
doi: 10.19277/bbr.18.2.267; [+] PDF version here; [+] Portuguese html here
Single versus mixed edge activators in caffeine-loaded transfersomes: physicochemical and cytotoxicity assessment
Íris Guerreiro 1, 2 #, Marta Rodrigues 3 #, Ana Sofia Fernandes 1, Catarina Rosado 1, Catarina Pereira-Leite 1, 4 *
1 CBIOS – Universidade Lusófona’s Research Center for Biosciences & Health Technologies, Av Campo Grande 376, 1749-024 Lisboa, Portugal;
2 Department of Biomedical Sciences, University of Alcalá, Ctra. Madrid-Barcelona Km. 33.600, 28871 Alcalá de Henares, Madrid, Spain;
3 Escola de Psicologia e Ciências da Vida, Universidade Lusófona de Humanidades e Tecnologias, Av Campo Grande 376, 1749-024 Lisboa, Portugal;
4 LAQV, REQUIMTE, Departamento de Ciências Químicas, Faculdade de Farmácia, Universidade do Porto, Rua de Jorge Viterbo Ferreira 228, 4050-313 Porto, Portugal
# These authors contributed equally to this work.
*corresponding author:
Abstract
The performance of transfersomes as nanovesicular systems to enhance the skin permeation of bioactive compounds may be modulated according to their composition of edge activators (EAs). Vesicle size, deformability, and encapsulation efficiency can be altered when using nonionic surfactants as EAs with opposing hydrophilic-lipophilic balance (HLB). Thus, this work aimed to assess the impact on the physicochemical properties and the in vitro cytotoxicity profile of transfersomal formulations composed of single or mixed EAs, with opposing HLB values. Transfersomes made of single or mixed nonionic surfactants (Tween® 80 and/or Span® 80) were prepared in the presence and absence of caffeine, used as a model hydrophilic compound. Single or mixed EAs-containing transfersomes displayed promising physicochemical properties for cutaneous applications and were found to be stable for one month of refrigerated storage. Moreover, all transfersomal formulations were compatible with a keratinocyte cell line upon 24 h treatment. Altogether, these preliminary data suggest that the use of mixed nonionic surfactants as EAs may be further explored to modulate the performance of transfersomes as skin permeation enhancers.
Keywords: Vesicular systems, nanotechnology, nonionic surfactants, caffeine
Received: 23/10/2021; Accepted: 08/12/2021
Introduction
Skin is a highly efficient barrier against the external environment, controlling the penetration of xenobiotics and microorganisms to maintain homeostasis. The outermost layer of the epidermis is the stratum corneum (SC), consisting of a matrix of layers of flattened corneocytes, extracellularly surrounded by multiple lipid bilayers (1,2). The unique structure of SC supports its primary function as cutaneous barrier, such that only a limited range of substances can permeate through skin, including substances with low molecular weight (<500 Da), relative lipophilicity (log P 1-3), and water solubility (3). Thus, the number of therapeutic agents amenable to transdermal administration is limited, triggering the development of different vesicular systems, such as liposomes, ethosomes, niosomes, and transfersomes (3-6), to enhance the permeation of bioactive compounds into the skin.
Transfersomes are highly elastic and deformable vesicles, and as such, they have been viewed as the most advantageous vesicular systems to enhance skin permeation (4,5). They were introduced by Cevc and Blume in 1992 (7) and are composed of phospholipids intercalated with edge activators (EAs) (4,5). The incorporation of EAs in the formulation of transfersomes provides their most important characteristic - ultra-deformability - as EAs act as destabilizers of the phospholipid bilayer by reducing interfacial tension (8). The ultra-elasticity of transfersomes allows them to deform and permeate through skin pores 5 to 10 times smaller than their size without losing their structure (3), and thus able to transport bioactive compounds to deeper skin layers. Transfersomes can be loaded with hydro- or lipophilic molecules with a wide range of molecular weights (200-106 Da). Thus, they have been explored for encapsulation of diverse therapeutic agents, including antioxidant, anticancer, anti-inflammatory, analgesic, anesthetic, antidiabetic, and antimicrobial compounds (5).
The performance of transfersomes as permeation enhancers of bioactive compounds depends on the phospholipid:EA ratio and the chosen EA (4,5).Various EAs have been explored to prepare transfersomes, in particular, nonionic surfactants (Tween® 80 and Span® 80) and bile acids (sodium deoxycholate and sodium cholate) (9-12). The choice of phospholipid:EA ratio is crucial to control the vesicle size and drug loading capacities, as recently reviewed (4,5). In fact, this parameter should be optimized, preferably by quality-by-design strategies, as excessive amounts of EA (> 15%) may lead to vesicle-to-micelle transitions (11). Moreover, the selection of EA in the preparation of transfersomes is a key factor to modulate their vesicle size and encapsulation efficiency. Considering nonionic surfactants, hydrophilic compounds may be more efficiently encapsulated using surfactants with high hydrophilic-lipophilic balance (HLB), while surfactants with low HLB values seem to better encapsulate lipophilic molecules (5). Moreover, the lower the HLB of nonionic surfactants, the higher the vesicle size (9) and the lower the vesicle deformability (10), which may ultimately reduce skin permeation. Altogether, these data indicate that modulating the HLB values by using mixtures of EAs may be a valuable strategy to optimize the performance of transfersomes.
In this context, this preliminary study aimed to evaluate the impact on the physicochemical properties and the in vitro cytotoxicity profile of transfersomes composed of single or mixed EAs with opposing HLB values. A pre-optimized formulation, using a quality-by-design approach, made of Tween® 80 (HLB=15) was the starting point for this work (13). The present study continued with EAs replaced and/or mixed with Span® 80 (HLB=4.3) . The bioactive molecule chosen to be encapsulated in the prepared transfersomes was caffeine, as it has been widely used as hydrophilic model compound in dermal safety studies (14). Moreover, its antioxidant and lipolytic activities support its extensive use in cutaneous formulations (15). To our knowledge, this is the first report on the physicochemical characterization and in vitro cytotoxicity assessment of transfersomes prepared with mixed EAs with opposing HLB values to load caffeine.
Materials and Methods
Materials
Caffeine was obtained from Fagron Ibérica (Terrassa, Spain). Lecithin from soybean was purchased from Alfa Aesar (Kandel, Germany). Tween® 80, potassium chloride, monobasic potassium phosphate, MTT (3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide) and trypsin were obtained from Sigma-Aldrich (Saint Louis, MO, USA). Span® 80 and DMSO (dimethyl sulfoxide) were purchased from Merck (Darmstadt, Germany). Chloroform and disodium hydrogen phosphate dihydrate were purchased from Scharlab S.L. (Sentmenat, Spain). Methanol was purchased from Carlo Erba Reagenti SpA (Rodano, Italy). SephadexTM G-25 medium was obtained from GE Healthcare Bio-sciences AB (Uppsala, Sweden). Sodium chloride was purchased from José M. Vaz Pereira SA (Benavente, Portugal). Low glucose DMEM (Dulbecco's Modified Eagle Medium) and FBS (fetal bovine serum) were purchased from Biowest (Nuaillé, France). Penicillin-streptomycin (pen/strep) was obtained from Grisp (Porto, Portugal). Phosphate-buffered saline (PBS) at pH 7.4 was prepared as previously described (13).
Preparation of transfersomes
Transfersomes were prepared using the lipid-film hydration method followed by sonication, as previously described (13). Seven formulations were prepared, with or without caffeine, consisting of lecithin (PC) and Tween® 80 and/or Span® 80 as EA, according to Table 1.
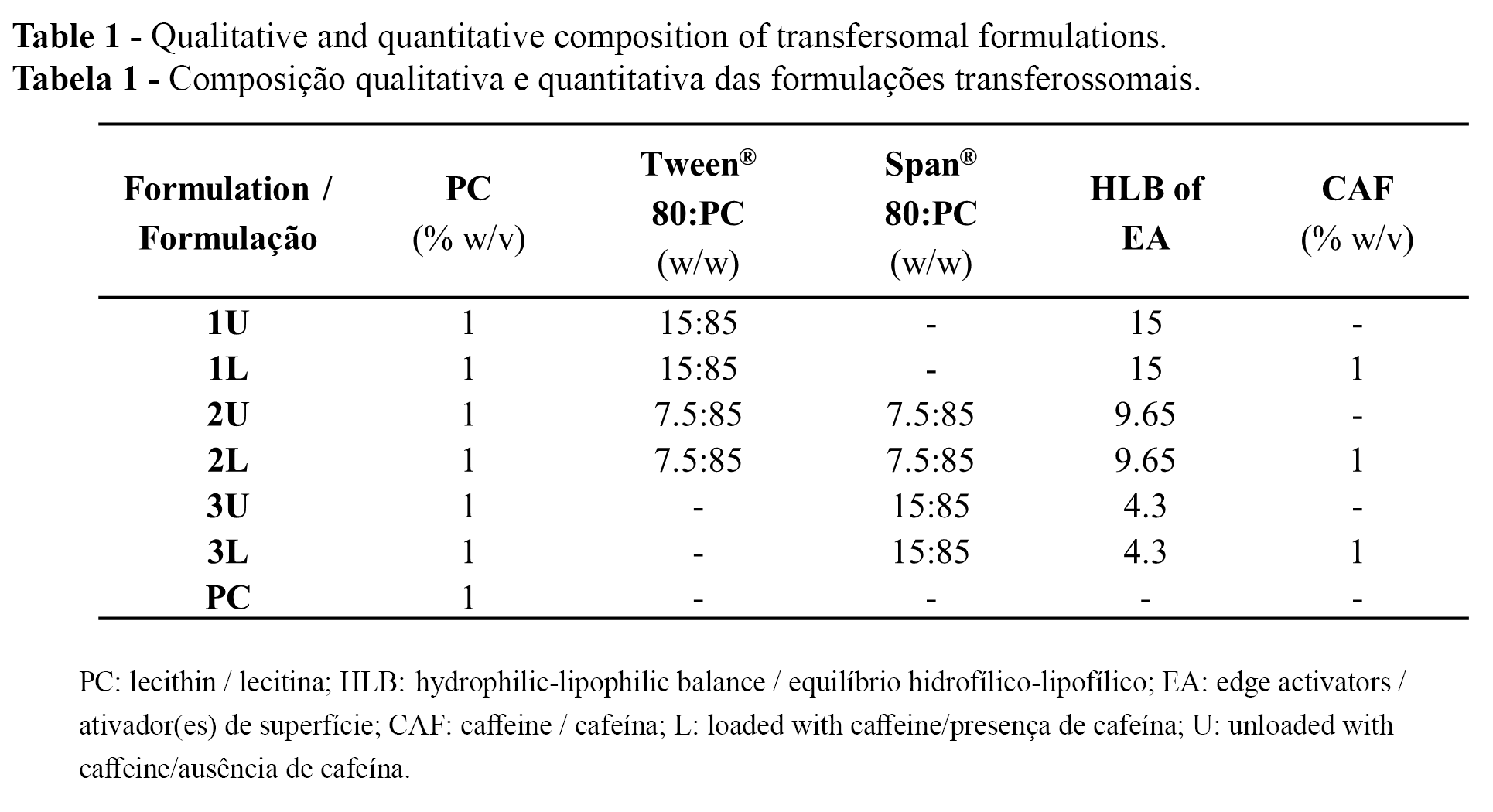
EA:PC films were obtained by dissolving the materials in chloroform:methanol (3:1, v/v) before solvent evaporation using a rotary evaporator (Model VV2000/VB2000, Heidolph Instruments, Schwabach, Germany) at 40 °C, 90 rpm, for 30 min. Traces of organic solvents were removed under vacuum for 2 h. The transfersomal formulations were prepared by hydrating the EA:PC films with PBS buffer or a 1% (w/v) caffeine buffered solution with vigorous vortexing. Finally, the formulations were sonicated (model Q125 sonicator, QSonica Sonicators, Newtown, CT, USA) at 50% amplitude for 10 min. .
Characterization of transfersomes
Immediately after preparation, the transfersomes were characterized according to their hydrodynamic diameter (Dh), polydispersity index (PDI), encapsulation efficiency (EE), and loading capacity (LC). The results were obtained from triplicate analysis of each formulation and reported as mean ± standard deviation (SD).
The Dh and PDI values of transfersomal formulations, diluted 1:20 with distilled water, were determined at room temperature (25 ± 2 °C) by dynamic light scattering measurements (DelsaTM Nano C equipment, Beckman Coulter, Inc., CA, USA).
The EE and LC of the transfersomes were analyzed using an indirect approach by the determination of the nonencapsulated fraction of caffeine using size exclusion chromatography, as previously described (13), with some modifications. A 500 μl aliquot of each formulation was applied to prepared SephadexTM G-25 medium (stationary phase). Following elution of the caffeine-encapsulated fractions (confirmed by visual analysis) with PBS (mobile phase), the nonencapsulated fraction of caffeine was collected for 30 min and the collected volume was recorded for accurate calculation of the dilution factor (collected volume/500 μl).
The concentration of caffeine in the nonencapsulated fraction was determined by UV-Vis spectroscopy (Evolution® 300, Thermo Scientific, Hertfordshire, England) using a calibration curve and considering the dilution factor. Six solutions of caffeine over a concentration range of 0-25 µg/ml were prepared in PBS to establish the concentration curve. The absorption spectrum (200-350 nm, 600 nm/min) of each solution was likewise obtained by UV/Vis spectroscopy. The calibration curve of caffeine (y=0.0539x-0.0077, R2=0.9991) was then determined considering the absorbance of caffeine at the absorption maximum wavelength (273 nm) as a function of caffeine concentration (µg/ml).
EE and LC values, represented as percentage (%), were calculated according to Equations 1 and 2, respectively:
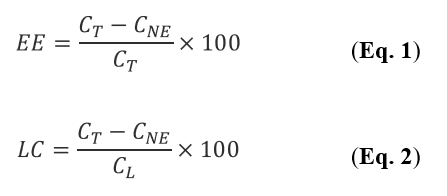
where CT represents the total concentration of caffeine, CNE the concentration of nonencapsulated caffeine, and CL the total concentration of PC.
Stability studies
The formulations were stored at 5 ± 2 °C for two months. The stability of Dh and PDI values of stored transfersomes was evaluated at different time points (Day 23, 30, and 60) and compared to the values obtained with freshly made formulations (Day 0). These parameters were evaluated as described above.
In vitro cytotoxicity assessment
Cell viability studies were performed using the HaCat cell line, representative of human keratinocytes, which was cultured in low glucose DMEM, supplemented with 10% FBS and 1% pen/strep and was kept at 37 °C under a humidified air atmosphere with 5% CO2.
The MTT reduction method was used to assess the cytotoxicity of the transfersomal formulations, in line with previous publications (16,17). Briefly, HaCat cells were seeded (6x103 cells/well, 200 µl of supplemented DMEM) in 96-well plates and were allowed to incubate for 24 h. After that, cells were treated for 24 h with a) control solutions, namely PBS or DMSO (5%, v/v) as negative and positive control (respectively); b) each transfersomal formulation diluted 1:100 and 1:200 in PBS, corresponding to caffeine concentrations of 515.7 and 257.9 µM (respectively); and c) buffered solutions of each individual component of the formulations, considering the quantitative composition of the formulations and the applied dilution factors. Afterwards, cells were washed with PBS and 200 µl of MTT solutions (0.5 mg/ml) in supplemented DMEM was added to each well, followed by an incubation period of 4 h. After another wash with PBS, 200 µl of DMSO were added to each well to dissolve the formazan crystals. Finally, the absorption values, at 595 nm, of each well were acquired using a microplate photometer (Thermo ScientificTM MultiskanTM FC). The absorption of PBS-treated cells was used as reference, representing 100% cell viability. Results were obtained from quadruplicates of each condition in two independent assays and are presented as mean ± SD.
Statistical analysis
All data were statistically analyzed using GraphPad Prism 8.0.2 (GraphPad Software, San Diego, California, USA). Physicochemical characterization and cell viability data were analyzed through unilateral variance analysis test (One-way ANOVA), followed by Turkey’s or Dunnett’s multiple comparison (respectively). Results regarding the stability studies were analyzed through bilateral variance analysis test (Two-way ANOVA), followed by Tukey’s multiple comparison. Differences were considered as statistically significant for p values under 0.05 (p<0.05).
Results and Discussion
Characterization of transfersomal formulations
The impact of using single or mixed EAs, namely Tween® 80 (1), Tween® 80:Span® 80 1:1 (2) or Span® 80 (3), to prepare transfersomes in the absence (U) and presence of caffeine (L) was evaluated in terms of Dh, PDI, EE, and LC. The results are summarised in Figure 1.
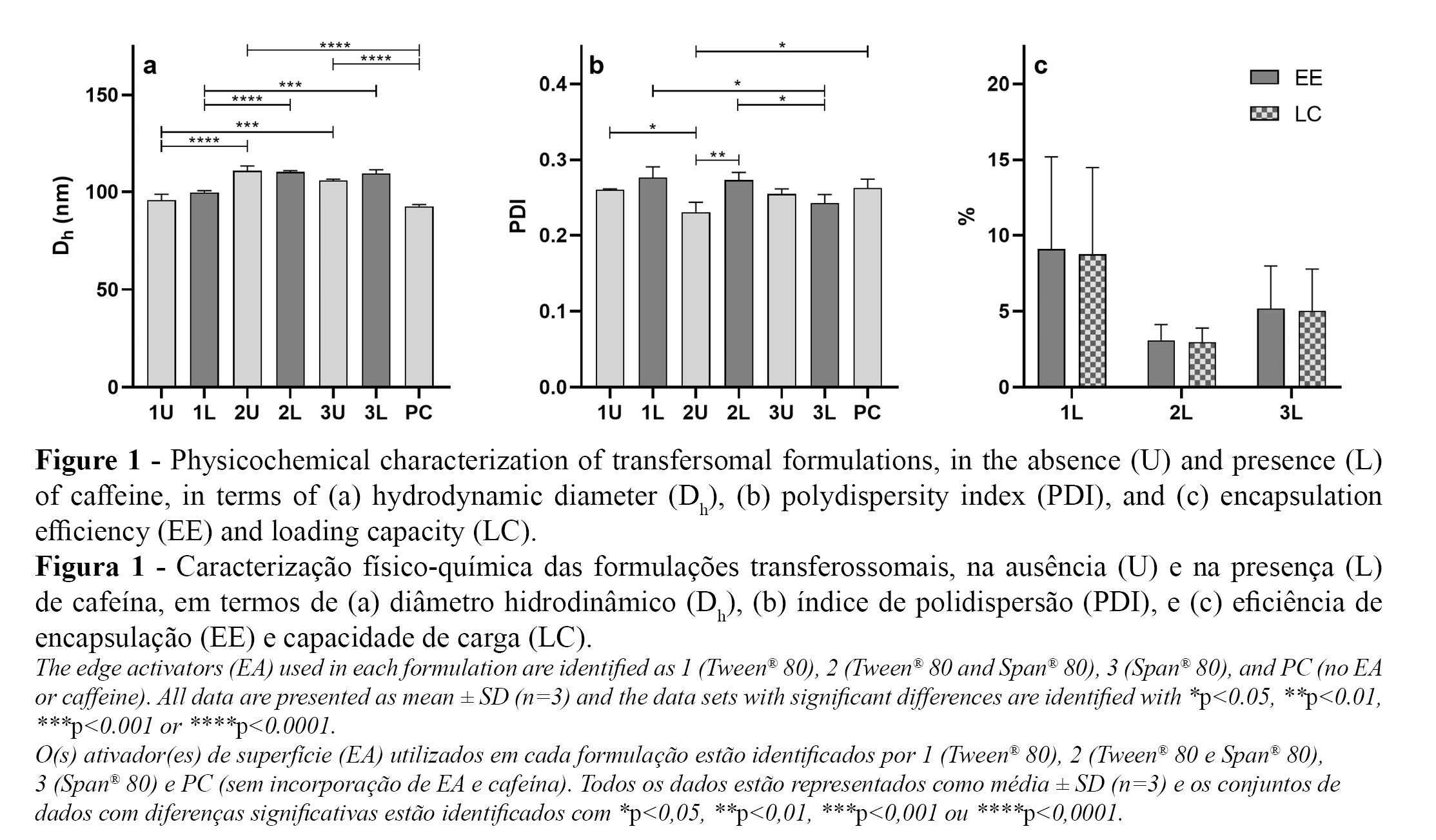
Regarding Dh data, all formulations have average diameters between 93 and 111 nm, which is a suitable range for transcutaneous application. In fact, previous studies indicate that transfersomes smaller than 300 nm are highly deformable and able to penetrate to deeper layers of the skin (4) and that the smaller the vesicle size, the greater its penetration into the skin (8, 18).
As shown in Figure 1a, the incorporation of caffeine did not change the size of transfersomes regardless of the type of EA used (1U-1L, 2U-2L, and 3U-3L comparisons). On the other hand, the size of the transfersomes varied according to the type of EA used both in the absence and presence of caffeine. In fact, using Tween® 80 as EA (1U or 1L) yielded smaller transfersomes than those prepared with the mixture of Tween® 80 and Span® 80 (2U or 2L) or with Span® 80 alone (3U or 3L). The significant increase of Dh values caused by the incorporation of Span® 80 was also observed in comparison with the PC formulation (2U-PC and 3U-PC comparisons), prepared in the absence of EAs. These results are in agreement with previously published results (9), as the increase in vesicle size may be related to the affinity of the surfactant for the phospholipid, with Span® 80 (HLB=4.3) having a higher affinity for PC, as it is more hydrophobic than Tween® 80 (HLB=15) (10).
The PDI values of transfersomal formulations was also evaluated (Figure 1b), and the average PDI values ranged between 0.23 and 0.28. It is noteworthy that smaller values of PDI in the absence of caffeine were obtained by preparing transfersomes with a mixture of Tween® 80 and Span® 80 (PDI(2U)=0.23±0.01). In contrast, in the presence of caffeine, the uniformity of size distribution was superior for transfersomes prepared with Span® 80 (PDI(3L)=0.24±0.01). Despite the small differences found in PDI values, the gathered data indicate that all transfersomal formulations are composed of monodisperse populations of vesicles, as PDI values lower than 0.3 are considered acceptable regarding the uniformity of vesicle size (19).
Concerning EE and LC of the prepared transfersomes, the average values ranged between 3% and 9%, with no significant differences according to the type of EAs used (Figure 1c). These results suggest that the amount of caffeine added exceeded the carrying capacity of the vesicles, so a decrease in the caffeine concentration and/or an increase in the concentration of excipients could potentially increase the EE and LC of these transfersomes in future studies. Due to the hydrophilic character of caffeine, its encapsulation will likely depend on the water content of the core of vesicles, which is directly related to number of vesicles in solution, thereby depending on the phospholipid concentration used to prepare the formulations (20). This hypothesis is in line with the results of Colletier et al. (21) who reported improvement of the EE of acetylcholinesterase by enhancing the phospholipid concentration used in liposome formulations.
Storage stability of transfersomal formulations
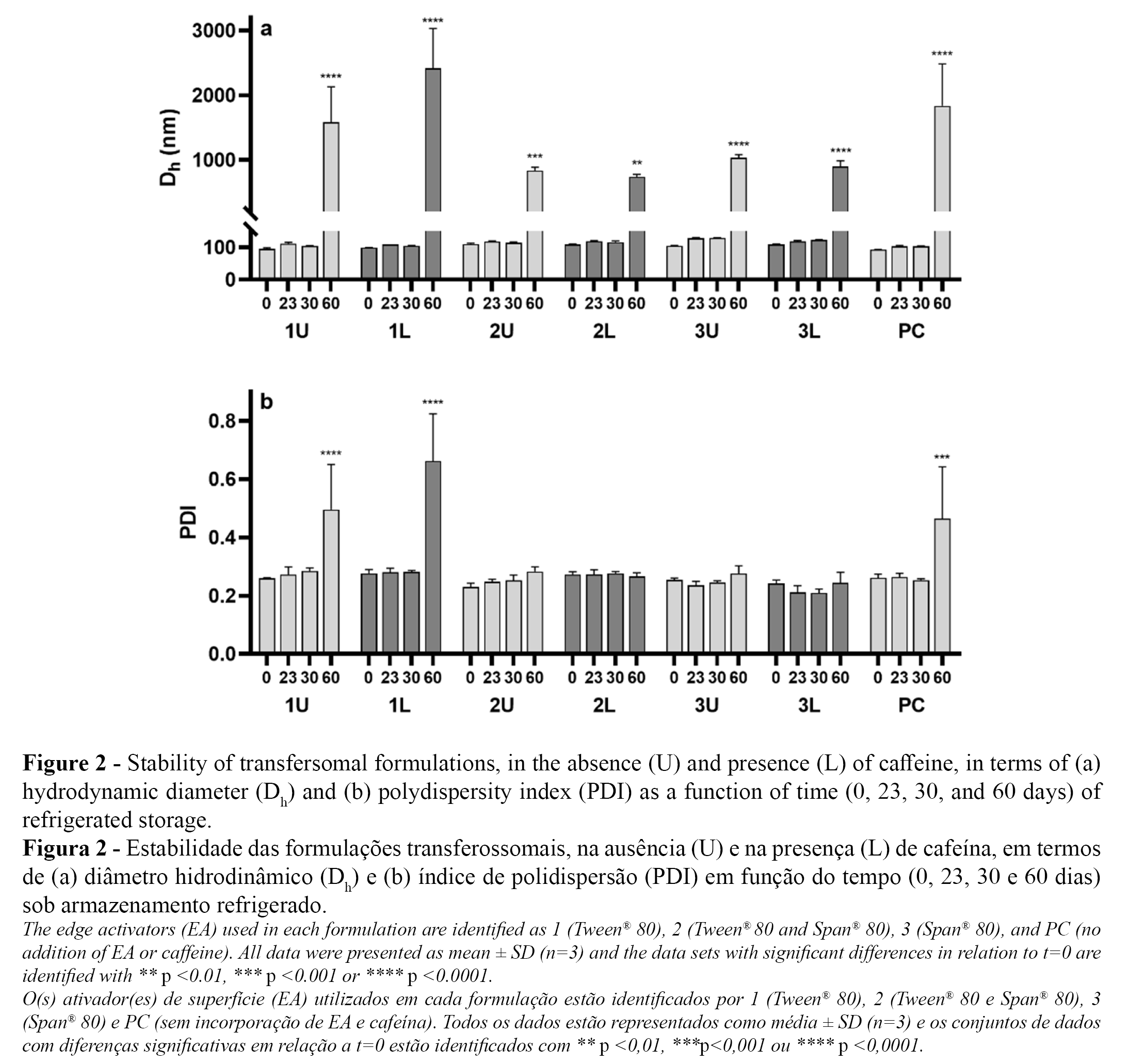
The physicochemical stability of the transfersomal formulations stored at 5 ± 2 °C was evaluated for two months by analyzing Dh and PDI of the transfersomes as a function of time (Figure 2). It is noteworthy that the properties of the formulations remained stable for one month. However, the diameter of the transfersomes significantly increased after two months in all cases, with a concomitant loss of vesicle size homogeneity (increased PDI) in the case of the 1U, 1L, and PC formulations. The increase in Dh values over time may be related to vesicle aggregation, that is more likely to occur when the surface charge of vesicles is close to neutrality (4,22). This may be the case in our study, since the main component of the prepared transfersomes is lecithin, a zwitterionic phospholipid. Thus, it would be of interest to evaluate the zeta potential of these vesicular systems in future studies to better understand the role of superficial charge on the aggregation phenomenon of these formulations.
In vitro cytotoxicity assessment of transfersomal formulations
The cytotoxicity potential of transfersomal formulations prepared with single or mixed EAs, in the absence and presence of caffeine, was evaluated upon treatment of HaCat cells for 24 h using the MTT reduction method. The results collected for all formulations and all individual components of the formulations, after a 1:100 or 1:200 dilution in PBS, are presented in Figure 3. It is noteworthy that the treatment with the positive control (DMSO-treated cells) caused a significant reduction in cell viability compared to control cells (PBS-treated cells), as expected.
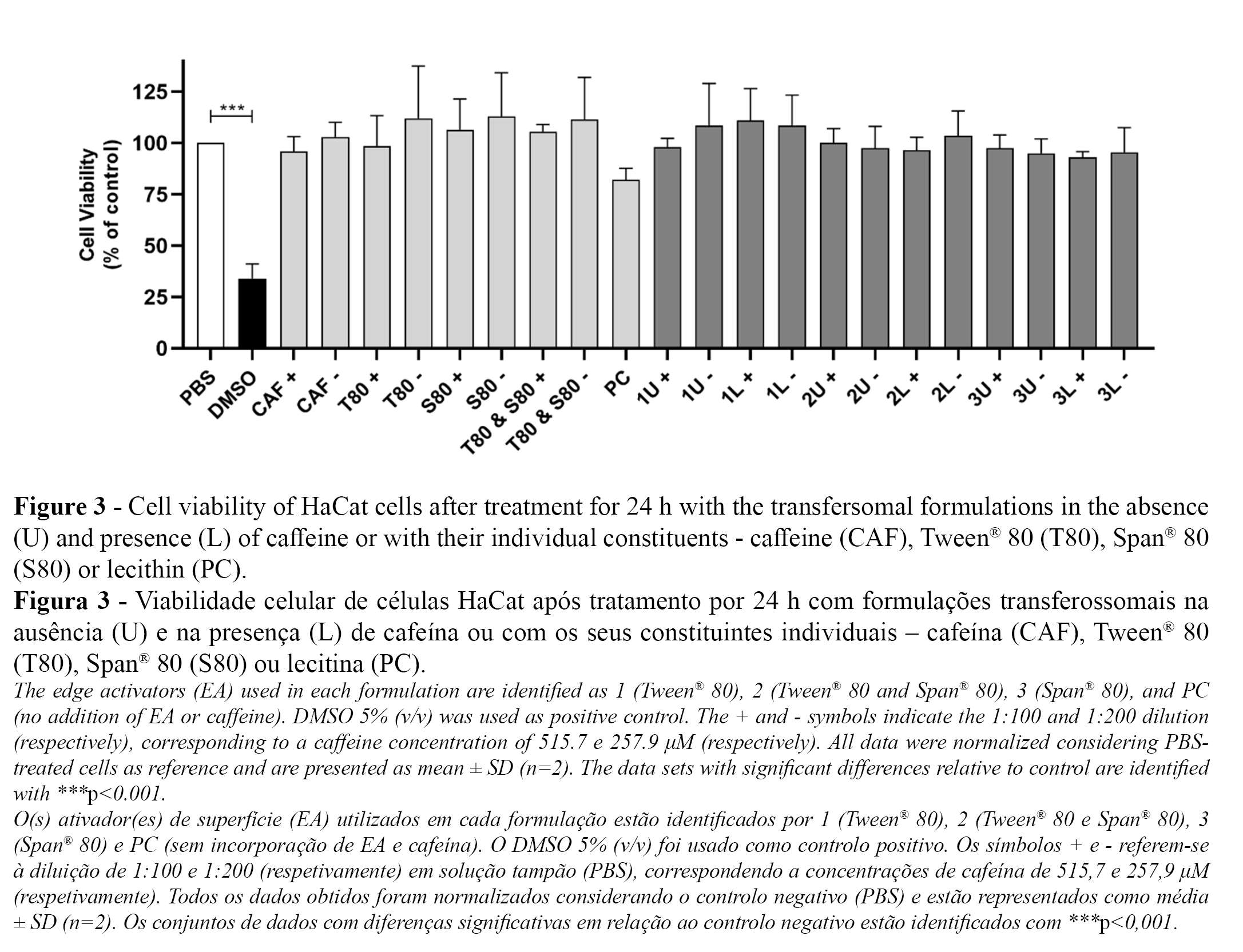
Human keratinocytes treated with encapsulated or nonencapsulated caffeine, at both concentrations under study (515.7 and 257.9 μM), did not show significant differences in cell viability when compared to control cells. These data are in agreement with previously reported studies showing that the treatment of HaCat cells with a caffeine concentration below 512 μM for 24 h does not affect the cellular viability (23, 24).
The incorporation of Tween® 80, Span® 80, or the mixture of both in transfersomes did not affect the cytotoxicity potential of the formulations. In addition, each component of the formulations (at both concentrations under study) did not significantly reduce the viability of HaCat cells. Once again, these results are in line with previous publications regarding the incorporation of Tween® 80 or Span® 80 in transfersomal formulations. In particular, no cytotoxicity was reported for Span® 80-containing transfersomes after treating HaCat cells up to 48 h (25), as well as for Tween® 80-containing transfersomes after treating mouse melanoma cells for 24 h (12). To our knowledge, this is the first report on the cytocompatibility of transfersomes composed of Tween® 80 and Span® 80, paving the way for the development of innovative transfersomal formulations made of mixed EAs.
Conclusion
In this exploratory work, we demonstrated that transfersomes composed of single or mixed nonionic surfactants as EAs display interesting physicochemical properties for cutaneous compound delivery. Moreover, these vesicular systems were stable for one month during refrigerated storage. Although the EE and LC values of the transfersomes must be further optimized in the future, the cell viability results were also very promising, as all formulations were compatible with human keratinocytes upon 24 h treatment at the studied concentrations. Altogether, this study indicates that the use of mixed nonionic surfactants as EAs may be a valuable strategy to modulate the performance of transfersomes. Further studies are ongoing to determine the best ratio between nonionic surfactants in order to improve the encapsulation efficiency and the skin permeation of these vesicular systems. The later property may be further improved with the incorporation of transfersomes in a semisolid formulation, such as a gel, as it may extend the retention time on the skin.
Authors Contributions Statement
CPL, ASF, and CR, conceptualization and study design; IG, MR, and CPL, experimental implementation; IG and CPL, data analysis; IG, MR, and CPL, drafting, editing and reviewing; IG, MR, and CPL, figures and graphics; CPL, ASF, and CR, supervision and final writing.
Funding
This study was supported by Fundação para a Ciência e a Tecnologia (FCT) through projects UIDB/04567/2020 and UIDP/04567/2020 to CBIOS and PhD grant 2020.07813.BD to I.G.
Conflict of Interests
The authors declare there are no financial and/or personal relationships that could present a potential conflict of interests.
References
- Uche, L. E., Gooris, G. S., Beddoes, C. M., & Bouwstra, J. A. (2019). New insight into phase behavior and permeability of skin lipid models based on sphingosine and phytosphingosine ceramides. Biochimica et Biophysica Acta - Biomembranes, 1861(7), 1317-1328. doi:10.1016/j.bbamem.2019.04.00
- van Smeden, J., & Bouwstra, J. A. (2016). Stratum Corneum Lipids: Their Role for the Skin Barrier Function in Healthy Subjects and Atopic Dermatitis Patients. Current Problems in Dermatologyl, 49, 8-26. doi:10.1159/000441540
- Zhou, X., Hao, Y., Yuan, L., Pradhan, S., Shrestha, K., Pradhan, O.,Hongjie, L., Li, W. (2018). Nano-formulations for transdermal drug delivery: A review. Chinese Chemical Letters 29(12), 1713-1724. doi:10.1016/j.cclet.2018.10.037
- Fernández-García, R., Lalatsa, A., Statts, L., Bolás-Fernández, F., Ballesteros, M. P., & Serrano, D. R. (2020). Transferosomes as nanocarriers for drugs across the skin: Quality by design from lab to industrial scale.International Journal of Pharmaceutics, 573,118817. doi:10.1016/j.ijpharm.2019.118817
- Opatha, S. A. T., Titapiwatanakun, V., & Chutoprapat, R. (2020). Transfersomes: A Promising Nanoencapsulation Technique for Transdermal Drug Delivery. Pharmaceutics, 12(9), 855. doi:10.3390/pharmaceutics12090855
- Roberts, M. S., Mohammed, Y., Pastore, M. N., Namjoshi, S., Yousef, S., Alinaghi, A., . . . Grice, J. E. (2017). Topical and cutaneous delivery using nanosystems.Journal of Controlled Release, 247, 86-105. doi:10.1016/j.jconrel.2016.12.022
- Cevc, G., & Blume, G. (1992). Lipid vesicles penetrate into intact skin owing to the transdermal osmotic gradients and hydration force. Biochimica et Biophysica Acta, 1104(1), 226-232. doi:10.1016/0005-2736(92)90154-e
- Cevc, G., Gebauer, D., Stieber, J., Schätzlein, A., & Blume, G. (1998). Ultraflexible vesicles, Transfersomes, have an extremely low pore penetration resistance and transport therapeutic amounts of insulin across the intact mammalian skin. Biochimica et Biophysica Acta, 1368(2), 201-215. doi:10.1016/s0005-2736(97)00177-6
- Ahmed, T. A. (2015). Preparation of transfersomes encapsulating sildenafil aimed for transdermal drug delivery: Plackett-Burman design and characterization.Journal of Liposome Research, 25(1), 1-10. doi:10.3109/08982104.2014.950276
- El Zaafarany, G. M., Awad, G. A., Holayel, S. M., & Mortada, N. D. (2010). Role of edge activators and surface charge in developing ultradeformable vesicles with enhanced skin delivery. International Journal of Pharmaceutics, 397(1-2), 164-172. doi:10.1016/j.ijpharm.2010.06.034
- Jangdey, M. S., Gupta, A., Saraf, S., & Saraf, S. (2017). Development and optimization of apigenin-loaded transfersomal system for skin cancer delivery: in vitro evaluation. Artificial Cells, Nanomedicine, and Biotechnology 45(7), 1452-1462. doi:10.1080/21691401.2016.1247850
- Wu, P. S., Li, Y. S., Kuo, Y. C., Tsai, S. J., & Lin, C. C. (2019). Preparation and Evaluation of Novel Transfersomes Combined with the Natural Antioxidant Resveratrol. Molecules, 24(3), 600. doi:10.3390/molecules24030600
- Pereira-Leite, C., & Ventura, C. (2020). Optimization of gallic acid-loaded transfersomes using a Box-Behnken factorial design. Biomedical and Biopharmaceutical Research, 17(2), 209-221. doi:10.19277/bbr.17.2.244
- Luo, L., & Lane, M. E. (2015). Topical and transdermal delivery of caffeine. International Journal of Pharmaceutics, 490(1-2), 155-164. doi:10.1016/j.ijpharm.2015.05.050
- Herman, A., & Herman, A. P. (2013). Caffeine's mechanisms of action and its cosmetic use. Skin Pharmacology and Physiology, 26(1), 8-14. doi:10.1159/000343174
- Caparica, R., Júlio, A., Araújo, M. E. M., Baby, A. R., Fonte, P., Costa, J. G., & Santos de Almeida, T. (2020). Anticancer Activity of Rutin and Its Combination with Ionic Liquids on Renal Cells. Biomolecules, 10(2). doi:10.3390/biom10020233
- Júlio, A., Caparica, R., Costa Lima, S. A., Fernandes, A. S., Rosado, C., Prazeres, D., Reis, S., Santos de Almeida, T., & Fonte, P. (2019). Ionic Liquid-Polymer Nanoparticle Hybrid Systems as New Tools to Deliver Poorly Soluble Drugs. Nanomaterials (Basel), 9(8). doi:10.3390/nano9081148
- Geusens, B., Van Gele, M., Braat, S., De Smedt, S. C., Stuart, M. C. A., Prow, T. W., Sanchez, W., Roberts, M.S., Sanders, N.N., Lambert, J. (2010). Flexible Nanosomes (SECosomes) Enable Efficient siRNA Delivery in Cultured Primary Skin Cells and in the Viable Epidermis of Ex Vivo Human Skin. Advanced Functional Materials, 20(23), 4077-4090. doi:10.1002/adfm.201000484
- Danaei, M., Dehghankhold, M., Ataei, S., Hasanzadeh Davarani, F., Javanmard, R., Dokhani, A., Mozafari, M. R. (2018). Impact of Particle Size and Polydispersity Index on the Clinical Applications of Lipidic Nanocarrier Systems. Pharmaceutics, 10(2), 57. doi:10.3390/pharmaceutics10020057
- Abd, E., Gomes, J., Sales, C. C., Yousef, S., Forouz, F., Telaprolu, K. C., Roberts, M. S., Grice, J. E., Lopes, P. S., Leite-Silva, V. R., & Andréo-Filho, N. (2021). Deformable liposomes as enhancer of caffeine penetration through human skin in a Franz diffusion cell test.International Journal of Cosmetic Science, 43(1), 1–10. https://doi.org/10.1111/ics.12659
- Colletier, J. P., Chaize, B., Winterhalter, M., & Fournier, D. (2002). Protein encapsulation in liposomes: efficiency depends on interactions between protein and phospholipid bilayer. BMC Biotechnology, 2, 9. doi:10.1186/1472-6750-2-9
- Kapoor, B., Gupta, R., Gulati, M., Singh, S. K., Khursheed, R., & Gupta, M. (2019). The Why, Where, Who, How, and What of the vesicular delivery systems. Advances in Colloid and Interface Science 271,101985. doi:10.1016/j.cis.2019.07.006
- Ojeh, N., Stojadinovic, O., Pastar, I., Sawaya, A., Yin, N., & Tomic-Canic, M. (2016). The effects of caffeine on wound healing.International Wound Journal, 13(5), 605-613. doi:10.1111/iwj.12327
- Xu, H., Gan, C., Gao, Z., Huang, Y., Wu, S., Zhang, D., . . . Sheng, J. (2020). Caffeine Targets SIRT3 to Enhance SOD2 Activity in Mitochondria.Frontiers in Cell and Developmental Biology, 8,822. doi:10.3389/fcell.2020.00822
- Volkwyn, M. (2017). In Vitro Biocompatibility of Transferosomes, Ethosomes and Transethosomes. North-West University, Potchefstroom Campus, Retrieved from https://books.google.pt/books?id=Thv_ygEACAAJ
