![]()
Biomedical Sciences, Biomed Biopharm Res., 2021; 18(1):15-24
doi: 10.19277/bbr.18.1.258; download pdf version [+] here
Body composition assessment of vegetarian-vegan and omnivore young women – an exploratory study
Cíntia Ferreira-Pêgo 1*, Rejane Giacomelli Tavares 1, Sofia Lopes 2, Tatiana Fontes 1, Luís Monteiro Rodrigues 1
1CBIOS – Universidade Lusofona’s Research Center for Biosciences & Health Technologies, Campo Grande 376, 1749-024 Lisboa, Portugal; 2School of Health Sciences and Technologies, Universidade Lusófona de Humanidades e Tecnologias, Lisboa, Portugal
*corresponding author:
Abstract
Diet is commonly accepted as a determinant of body composition, especially when related to specific lifestyles. Vegetarian-vegan diets, which involve a reduction or elimination of animal product consumption, are believed to be more “healthy,” facilitating weight control and reducing the incidence and clinical course of different diseases, in particular those related to overweight and obesity. Global reviews and metanalysis on these issues, however, are still insufficient. Our preliminary approach addresses the total body composition differences among vegetarians-vegans and omnivorous individuals. This cross-sectional study involved ten healthy women, five vegetarian-vegan, and five omnivores (mean 28.10 years old). Body composition was assessed using a dual-energy x-ray absorptiometry (DXA Lunar Prodigy Advance - General Electric Healthcare®). Other general and sociodemographic variables were also collected by trained dietitians. Our results have shown that the vegetarian-vegan group had a non-significantly lower volume of all types of body mass (total bone, fat, lean, tissue, and fat-free) evaluated. Additionally, the vegetarian-vegan group presented higher values of visceral adipose tissue and subcutaneous adipose tissue (286.20 and 11138.40 cm3, respectively, p > 0.05) compared to the omnivore group. These differences will be further confirmed in subsequent studies.
Keywords: Body composition; visceral adipose tissue; subcutaneous adipose tissue; vegetarian-vegan diet; Dual-energy x-ray absorptiometry
Received: 13/05/2021; Accepted: 03/06/2021
Introduction
Diet seems to have a significant influence on the development of adiposity, obesity, and cardiometabolic diseases (1). It is also clear that excess body fat is an established risk factor for many disease conditions and premature death (2).
Plant-based diets such as vegetarianism and veganism are believed to reduce body weight because of the overall decreased caloric intake and increased thermogenesis. These diets are most simply defined by a reduction or elimination of the consumption of animal products and based on the consumption of grains, legumes, vegetables, fruits, and nuts (3). However, it should be noted that reductions in body weight do not necessarily result in reductions in adipose tissue neither directly translate into improved health outcomes (4). Nevertheless, the vegetarian diet is reported as being an effective means for the prevention and treatment of cardio-metabolic diseases (3). The Academy of Nutrition and Dietetics, the world’s largest organization of food and nutrition professionals founded in 1917, recognizes the health and nutritional benefits for the prevention and treatment of certain diseases potentially related to vegetarian-vegan diets (5). Healthy, properly planned vegetarian diets were described as effective for glycemic control while providing metabolic and cardiovascular benefits, including the control of atherosclerosis dyslipidemia and blood pressure (3). These cardio-metabolic benefits were reported to be greater with vegan than lacto-ovo-vegetarian diets (6). However, the body composition of vegetarian and vegan individuals has not been sufficiently studied, and commonly-used assessments of waist circumference, body weight, or Body Mass Index (BMI) do not reveal body composition nor fat distribution. Therefore, the main goal of the present study was to approach and compare the body composition - bone mass, fat mass, lean mass, tissue mass, fat-free mass, total mass, and visceral and subcutaneous adipose tissue - of young healthy adult women with different diet regimes (vegetarian-vegan vs. omnivore) by referenced methods.
Materials and Methods
Study design and participants
The present study was an observational, quantitative, and cross-sectional analysis designed to evaluate total body composition in vegetarian-vegan individuals and comparing it with omnivore diet participants.
A convenience sample of ten participants (five vegetarian-vegan, and five omnivores) all women presenting a mean age of 28.10 (SD: 6.94) years old were selected from the university’s student body. Participants were selected following previously defined inclusion/ non-inclusion criteria. Apart from gender, non-inclusion criteria included any kind of disease or health alteration, taking any sort of medication, being pregnant or breastfeeding, and being in the first week of their menstrual cycle. All participants agreed to participate in the study, giving their informed written consent. Procedures respected the principles of good clinical practice adopted for human research studies complying with good clinical practice ethical standards for human research (7). Participants’ socio-demographics (age, course year, residence, and other lifestyle habits) were obtained and a Food Frequency Questionnaire and a 3-day dietary recall were also collected for each participant.
Body composition assessment
Weight was measured on an electronic scale [0.1 kg (0.1-200 kg) accuracy], wearing light clothing and no shoes. Height was a self-reported variable used to calculate BMI by the formula [BMI = weight (kg)/height (m2)].
The Dual-energy x-ray absorptiometry (DXA Lunar Prodigy Advance - General Electric Healthcare®; Chicago, Illinois, USA) was used to measure bone mass, fat mass, lean mass, tissue mass, fat-free mass, total mass, and visceral and subcutaneous adipose tissue. Before each whole-body scan, DXA was calibrated according to the manufacturer’s instructions via a standard calibration block. Measurements were performed under at least four hours of fasting conditions and without exercise the previous 24 hours to ensure adequate hydration conditions. Participants removed shoes, socks, and all jewelry. Wearing underwear or close-fitting clothing with no metallic piecess, participants were instructed to lie supine on the scanning bed with hands by their sides, not touching the body. During all body scans, participants were asked to remain motionless, and Velcro straps were situated around the ankles and knees. All participants on the DXA scanning bed were positioned on the scanning bed by the same trained researcher. Scans lasted approximately 5 to 10 minutes. The researcher analyzed each scan to adjust software-determined regions of interest before producing the whole-body report.
Statistical analysis
Data were presented either as means and standard deviation (SD) for continuous variables or percentages and absolute frequencies for dichotomous variables. The normality of the variables was tested. As all followed a normal distribution, the distribution of the selected characteristics between groups was tested using χ٢ tests for categorical variables or Student’s t-tests for continuous variables. All statistical tests were two-tailed and the significance level was set at p <0.05. All analyses were performed using the SPSS software version 27.0 (SPSS Inc, Chicago, IL, USA).
Results
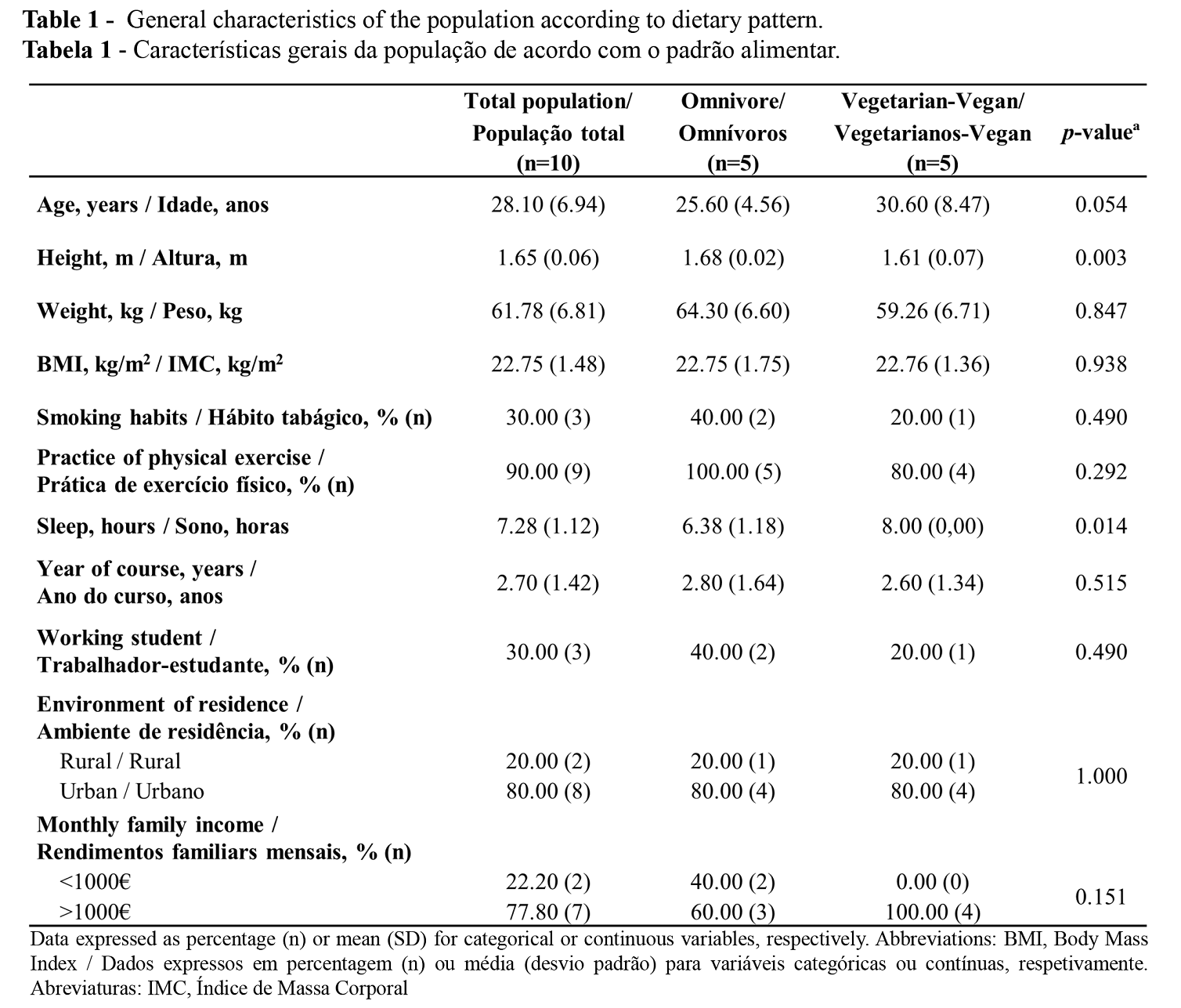
The general characteristics of the studied population according to its dietary pattern are summarized in Table 1. Omnivorous women were statistically taller than the vegan-vegetarian group, however, this difference does not affect BMI since no other differences in body weight were found. Sleeping hours were also statistically different between the groups analyzed, as participants following an animal-product diet slept fewer hours compared to the vegetarian group. No other statistically relevant differences were found.
The total population presented a mean bone mass of 2285.30 g, 18983.60 g of fat mass, 40532.60 g of lean mass, 59516.10 g of tissue mass, 42817.80 g of fat-free mass, and finally 63.40 kg of total body mass. Vegetarian-vegan women presented lower volume of all body mass types. However, none of these differences were statistically significant. The results are shown in Figure 1.
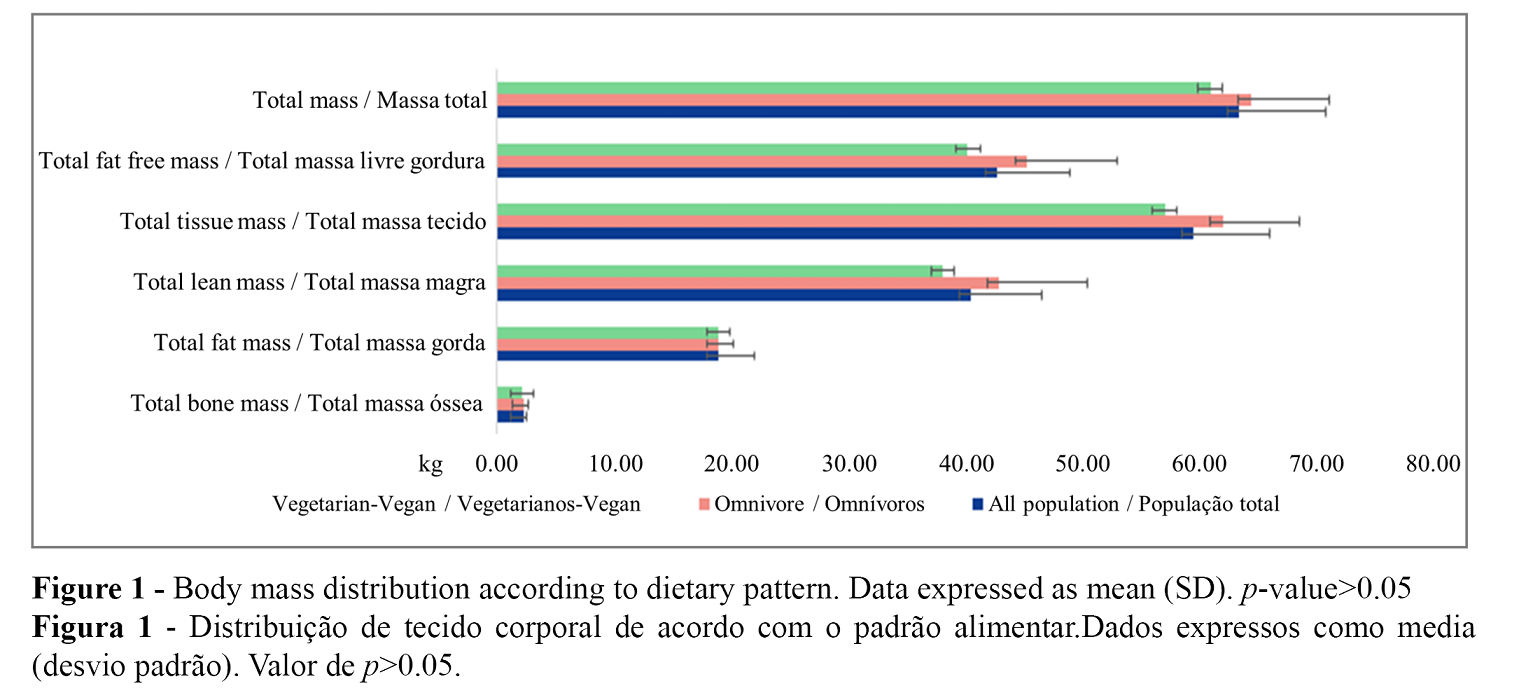
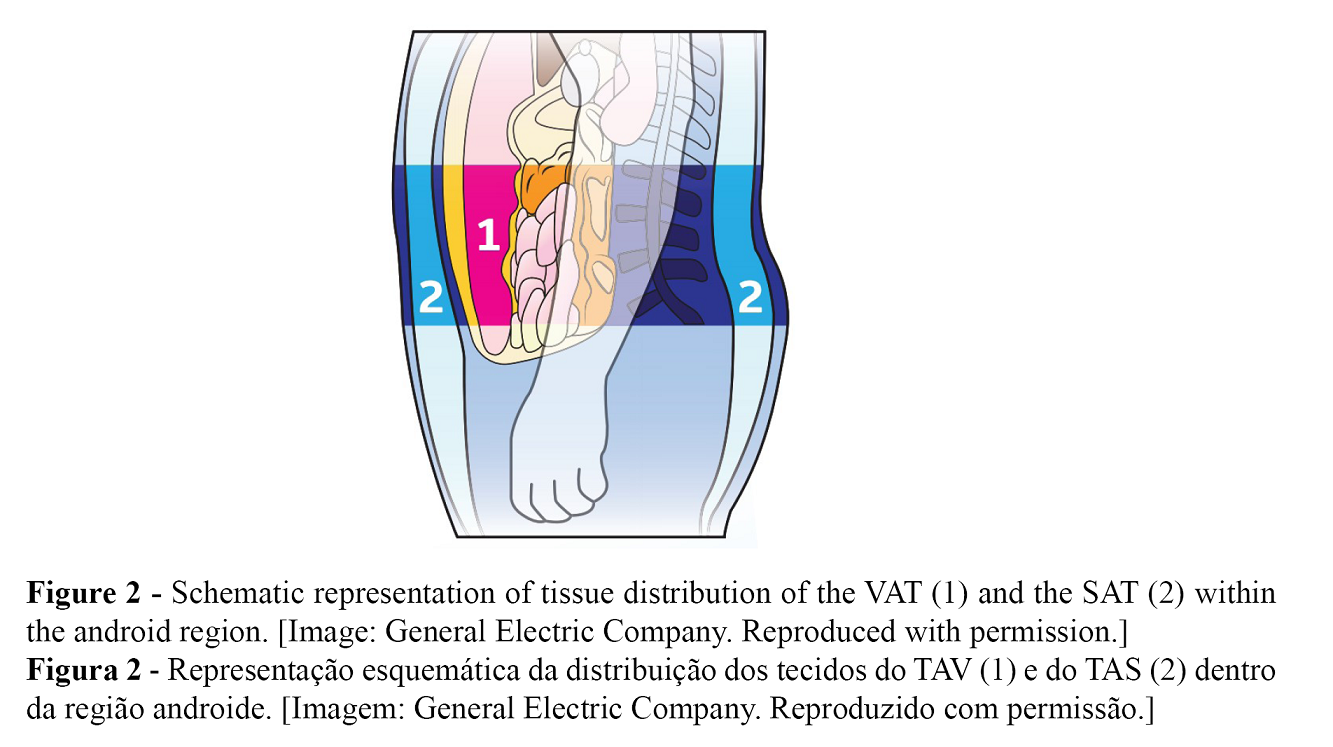
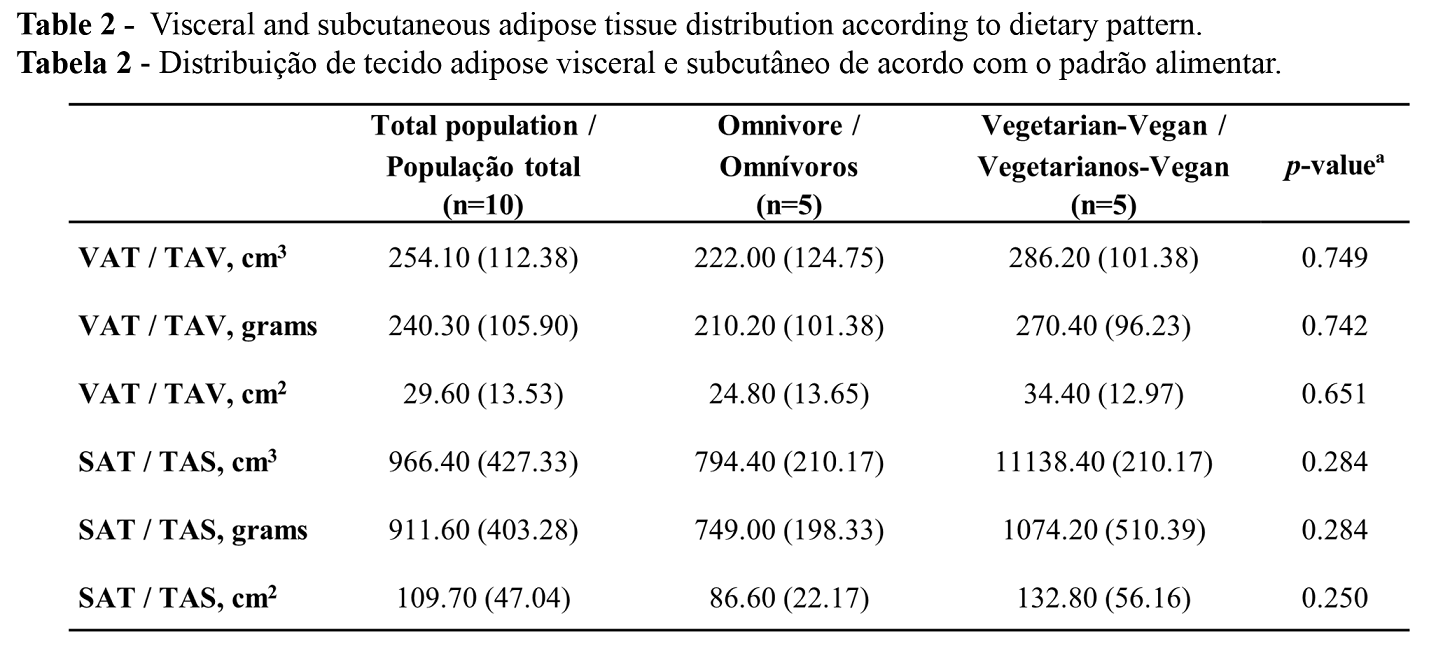
Figure 2 shows the areas of the adipose tissue calculation. Values regarding the visceral adipose tissue (VAT) and the subcutaneous adipose tissue (SAT) distribution for the entire studied population are summarized in Table 2, along with a comparison between vegetarian-vegan and omnivore participants. The total population presented a mean of 254.10 cm3, 240.30 g, and 29.60 cm2 of VAT, and 966.40 cm3, 911.60 g, and 109.70 cm2 of SAT. Vegetarian-vegan participants presented higher values of VAT and SAT (281.00 and 1025.00 cm3, respectively) compared to the omnivore group (219.17 and 831.00 cm3, respectively). None of these differences were statistically significant (p-value>0.05).
Discussion
Obesity and type 2 Diabetes Mellitus (T2DM) represent major risks to develop cardiovascular diseases (CVD), and insulin resistance related to adipose tissue (white and visceral) and pancreatic β-cells impairment are currently indicated as the primary mechanisms of T2DM (8), these links between obesity, insulin resistance, and CVD have recently drawn more attention to the importance of diet as part of lifestyle and thus a potentially effective way to help prevent these recognized major health burdens, associated or not to physical exercise and activity (9).
Plant-based diets have been described as reducing body fat via a variety of mechanisms, which cumulatively lead to reduced caloric intake and increased energy expenditure (4). These mechanisms might include the reduced caloric density of the overall diet and improved satiety, in part due to gut microbiota alterations (4). Additionally, increased insulin sensitivity, and a potential increase in white adipose tissue. contribute to increasing thermogenesis (4). Plant-based diets have also been consistently associated with reduced body weight in interventional trials (10,11). No matter this very small sample and exploratory character, our results have found no differences in BMI or weight between vegetarian and non-vegetarian participants. No statistical differences were observed regarding the fat mass distribution between those two groups. The vegetarian – vegan group depicted non-statistical higher VAT and SAT values, compared to the omnivore group. In recent years, excess VAT, also referred as visceral obesity. has been recognized as a major predictor of cardiometabolic disease and all-cause mortality independent of BMI and general obesity (12,13). Moreover, VAT is highly metabolically active and contributes to systemic inflammation, and has been assumed to be the common key element and driver of the cardiometabolic risk associated to the metabolic syndrome (14). Data available to date suggests a role for both VAT and SAT in chronic cardiometabolic disease (15). It has been argued that excess abdominal adipose tissue is a consequence of today’s modern, sedentary lifestyle patterns, including nutrition and dietary behaviour (13). Inherently, the relationship between dietary intake and health outcomes such as VAT and SAT is very complex, with interactions that are not captured by studying only single dietary components (16).
We might easily agree that no diet, independently, is more healthy than another. In all cases, the diet needs to be properly planned regarding its macro and micronutrient contents and the type of food products chosen (17).
To the best of our knowledge, this is the first published report detecting higher values of VAT and SAT with detailed body mass scanning in vegetarian-vegan young women and compared to a similar omnivore population. The reduced sample is an obvious constraint, limiting our interpretation. Still noninvasive imaging technologies such as DXA are validated to quantify the specific amounts of VAT and SAT in the body (18), and DXA analysis is regarded for that purpose as a “gold-standard”. Its accessibility and cost may explain the limited numbers of large scale epidemiological studies using this technique. Since SAT is the biggest reserve of VAT, these results should be further studied with special interest in healthy and normal weight and BMI individuals to better understand its relationship with diet and food group(s) consumption in healthy and non-healthy individuals.
Conclusion
This exploratory study revealed some (not statistically significant) differences between healthy volunteers following vegetarian-vegan and omnivorous dietary patterns. Vegetarian-vegan participants have shown consistently lower mass volumes (total bone mass, fat mass, lean mass, tissue mass, and fat-free mass) and higher levels of subcutaneous and visceral adipose tissue when compared with the omnivore group.
Authors Contributions Statement
C.F.-P., R.G.T, L.M.R conceptualization and study design; R.G.T., S.L., T.F. experimental implementation and data collection; C.F.-P. data analysis; C.F.-P., R.G.T., LMR drafting, editing and reviewing; C.F.-P. figures and graphics; C.F.-P., R.G.T., L.M.R supervision; C.F.-P., R.G.T., L.M.R. final writing.
Funding
Cíntia Ferreira Pêgo is funded by Foundation for Science and Technology (FCT) Scientific Employment Stimulus contract with the reference number CEEC/CBIOS/NUT/2018. This work is funded by national funds through FCT - Foundation for Science and Technology, I.P., under the UIDB/04567/2020 and UIDP/ 04567/2020 projects, and ALIES-COFAC - PADDICC2021.
Acknowledgements
The authors acknowledge all the participants.
Conflict of Interests
The senior editor involved in this manuscript's authorship had no participation in the review or decision process. All authors have stated that there are no financial and/or personal relationships that could represent a potential conflict of interest.
References
- Kaila, B., & Raman, M. (2008). Obesity: a review of pathogenesis and management strategies. Canadian journal of gastroenterology = Journal canadien de gastroenterologie, 22(1), 61–68. https://doi.org/10.1155/2008/609039.
- Ratjen, I., Morze, J., Enderle, J., Both, M., Borggrefe, J., Müller, H. P., Kassubek, J., Koch, M., & Lieb, W. (2020). Adherence to a plant-based diet in relation to adipose tissue volumes and liver fat content. The American journal of clinical nutrition, 112(2), 354–363. https://doi.org/10.1093/ajcn/nqaa119
- Kahleova, H., Levin, S., & Barnard, N. (2017). Cardio-Metabolic Benefits of Plant-Based Diets. Nutrients, 9(8), 848. https://doi.org/10.3390/nu9080848
- Najjar, R. S., & Feresin, R. G. (2019). Plant-Based Diets in the Reduction of Body Fat: Physiological Effects and Biochemical Insights. Nutrients, 11(11), 2712. https://doi.org/10.3390/nu11112712
- Melina, V., Craig, W., & Levin, S. (2016). Position of the Academy of Nutrition and Dietetics: Vegetarian Diets. Journal of the Academy of Nutrition and Dietetics, 116(12), 1970–1980. https://doi.org/10.1016/j.jand.2016.09.025
- Le, L. T., & Sabaté, J. (2014). Beyond meatless, the health effects of vegan diets: findings from the Adventist cohorts. Nutrients, 6(6), 2131–2147. https://doi.org/10.3390/nu6062131
- World Medical Association. WMA DECLARATION OF HELSINKI – ETHICAL PRINCIPLES FOR MEDICAL RESEARCH INVOLVING HUMAN SUBJECTS [Internet]. 2018 [cited 2021 Jun 2]. Available from: https://www.wma.net/policies-post/wma-declaration-of-helsinki-ethical-principles-for-medical-research-involving-human-subjects/
- Chait, A., & den Hartigh, L. J. (2020). Adipose Tissue Distribution, Inflammation and Its Metabolic Consequences, Including Diabetes and Cardiovascular Disease. Frontiers in cardiovascular medicine, 7,22. https://doi.org/10.3389/fcvm.2020.00022
- Longo, M., Zatterale, F., Naderi, J., Parrillo, L., Formisano, P., Raciti, G. A., Beguinot, F., & Miele, C. (2019). Adipose Tissue Dysfunction as Determinant of Obesity-Associated Metabolic Complications. International journal of molecular sciences, 20(9), 2358. https://doi.org/10.3390/ijms20092358
- Barnard, N. D., Levin, S. M., & Yokoyama, Y. (2015). A systematic review and meta-analysis of changes in body weight in clinical trials of vegetarian diets. Journal of the Academy of Nutrition and Dietetics, 115(6), 954–969. https://doi.org/10.1016/j.jand.2014.11.016.
- Huang, R. Y., Huang, C. C., Hu, F. B., & Chavarro, J. E. (2016). Vegetarian Diets and Weight Reduction: a Meta-Analysis of Randomized Controlled Trials. Journal of general internal medicine, 31(1), 109–116. https://doi.org/10.1007/s11606-015-3390-7
- Kuk, J. L., Katzmarzyk, P. T., Nichaman, M. Z., Church, T. S., Blair, S. N., & Ross, R. (2006). Visceral fat is an independent predictor of all-cause mortality in men. Obesity (Silver Spring, Md.), 14(2), 336–341. https://doi.org/10.1038/oby.2006.43
- Tchernof, A., & Després, J. P. (2013). Pathophysiology of human visceral obesity: an update. Physiological reviews, 93(1), 359–404. https://doi.org/10.1152/physrev.00033.2011
- Ibrahim M. M. (2010). Subcutaneous and visceral adipose tissue: structural and functional differences. Obesity reviews : an official journal of the International Association for the Study of Obesity, 11(1), 11–18. https://doi.org/10.1111/j.1467-789X.2009.00623.x
- Abate, N., & Chandalia, M. (2012). Role of subcutaneous adipose tissue in metabolic complications of obesity. Metabolic syndrome and related disorders, 10(5), 319–320. https://doi.org/10.1089/met.2012.1502
- Fischer, K., Pick, J. A., Moewes, D., & Nöthlings, U. (2015). Qualitative aspects of diet affecting visceral and subcutaneous abdominal adipose tissue: a systematic review of observational and controlled intervention studies. Nutrition reviews, 73(4), 191–215. https://doi.org/10.1093/nutrit/nuu006
- Kahleova, H., Petersen, K. F., Shulman, G. I., Alwarith, J., Rembert, E., Tura, A., Hill, M., Holubkov, R., & Barnard, N. D. (2020). Effect of a Low-Fat Vegan Diet on Body Weight, Insulin Sensitivity, Postprandial Metabolism, and Intramyocellular and Hepatocellular Lipid Levels in Overweight Adults: A Randomized Clinical Trial. JAMA network open, 3(11), e2025454.https://doi.org/10.1001/jamanetworkopen.2020.25454/
- Shuster, A., Patlas, M., Pinthus, J. H., & Mourtzakis, M. (2012). The clinical importance of visceral adiposity: a critical review of methods for visceral adipose tissue analysis. The British journal of radiology, 85(1009), 1–10. https://doi.org/10.1259/bjr/38447238
